October is Breast Cancer Awareness Month
Let’s learn the facts:
- 1 in 8 U.S. women will develop invasive breast cancer over the course of her lifetime
- In 2020, an estimated 276,480 new cases of invasive breast cancer are expected to be diagnosed in women in the U.S., along with 48,530 new cases of non-invasive (in situ) breast cancer
- 2,620 new cases of invasive breast cancer are expected to be diagnosed in men in 2020. A man’s lifetime risk of breast cancer is about 1 in 883.
- After skin cancer, breast cancer is the most commonly diagnosed cancer among American women
- A woman’s risk of breast cancer nearly doubles if she has a first-degree relative (mother, sister, daughter) who has been diagnosed with breast cancer
- 85% of breast cancers occur in women who have no family history of breast cancer, due to genetic mutations that happen as a result of the aging process and life in general, rather than inherited mutations
- The most significant risk factors for breast cancer are sex (being a woman) and age (growing older)

How often should you do breast self-examinations?
Once a month, usually 2-3 days after your period has ended. The more regularly you perform them, the more aware you’ll be of your own anatomy making it easier to detect an abnormality. Self-examination combined with regular physical examinations can be a helpful screening tool. Don’t fret if you feel something abnormal, monitor for changes and/or call your doctor for follow-up.

When should you start getting mammograms?
According to the ACS (American Cancer Society), women may begin screening with mammography at age 40-44 and should get mammograms every year age 45-54. Once 55 and older, mammograms can be performed every other year.
According to the USPTF (United States Preventative Task Force), women should have biennial screening ages 50-74 but a significant family history my warrant screening in the 40s.
Most providers begin screenings at age 40 and will begin sooner if their patient has a significant family history.
Here is my comparison chart from my Let’s Talk Cancer Screenings post according to the ACS and USPTF. Check out the post for details on the top cancers in our world today and when/how to screen.
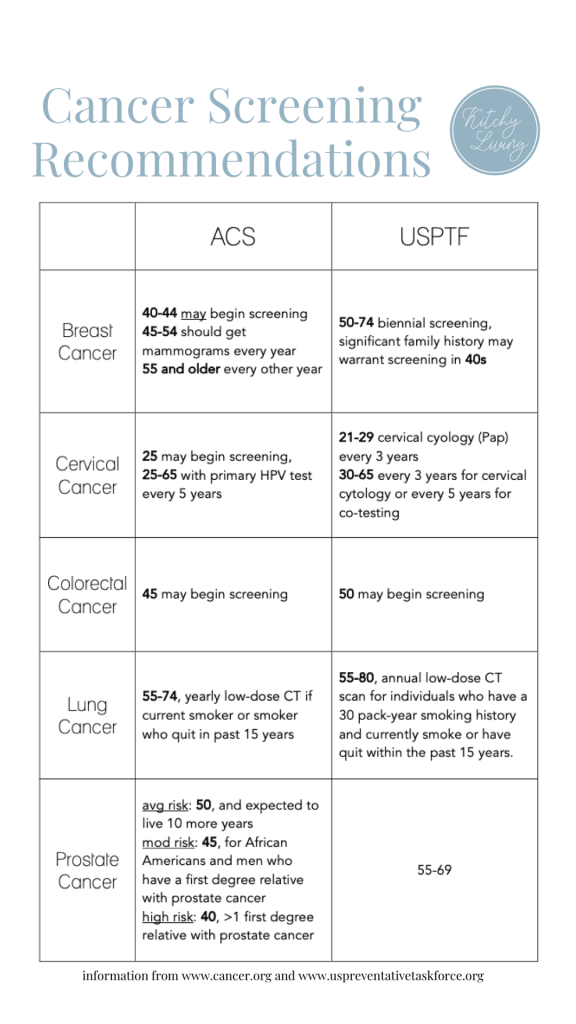
What are some of the breast cancer screening and diagnostic tools?
Breast cancer related tools can be broken down into three different categories:
1. Screening tools: routine tools used to find cancer early in the general population
EX: Breast self-exam, mammogram, blood marker tests (family history),
2. Diagnostic tools: the next step in management/workup of suspected breast cancer to help gather information and guide decision-making and treatment
EX: Breast MRI, molecular breast imaging (scintimammography), ultrasound, biopsy, fluorescence in situ hybridization (FISH)
3. Monitoring tools: after a confirmed diagnosis of breast cancer, these tools will be used to monitor treatment progress
EX: DEXA bones scan, CT scan, chest xray, breast MRI, PET scans
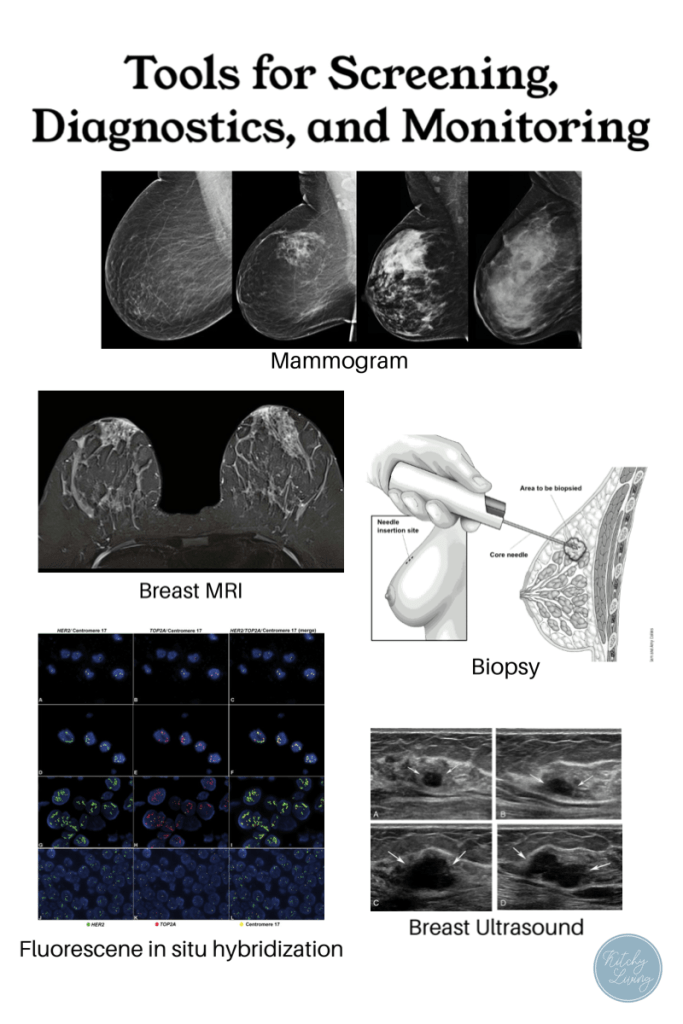
What are some of the blood marker tests?
CA 15.3, TRU-QUANT or CA 27.29, CA125, CEA, and circulating tumor cells.
If you do not have an OB-GYN and are a woman of reproductive age, I cannot implore you enough to find a provider. Routine physical exams help save lives, not to mention routine screenings like pap smears. Do some research, find a group you like, and make the call. Your body deserves routine care for the sake of your health, longevity, and overall quality of life.
This infographic is a great illustration of some abnormal breast changes that require follow-up with your doctor. Changes like thickness, dimpling, nipple crust, redness or warmth, new fluid production, skin sores, bumps, veins, retracted nipples, abnormal shape, orange-peel skin, and hard lumps.
Never be afraid to contact your doctor or medical provider if you think you’ve found something concerning. It never hurts to get checked out!

For More Information:
American Breast Cancer Foundation
American Cancer Society
Breast Cancer Research Foundation
BreastCancer.org
National Breast Cancer Foundation, Inc.
Susan G. Komen
I hope you learned something today!







Leave a comment